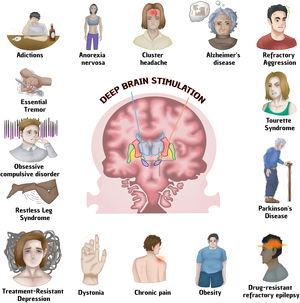
Introduction
Deep brain stimulation (DBS) is a neurosurgical technique that modulates neural circuits through electrical impulses. Initially developed for motor disorders such as Parkinson’s disease, its use has expanded to neuropsychiatric conditions, including treatment-resistant schizophrenia, obsessive-compulsive disorder (OCD), and chronic anorexia nervosa, with promising results. However, challenges remain regarding treatment personalization, identification of anatomical targets, and understanding its mechanisms of action.
Objective
To assess the effectiveness, safety, and technical factors associated with DBS in neuropsychiatric disorders through a systematic review of the available scientific literature.
Methods
A systematic review was conducted following PRISMA guidelines. Controlled clinical trials, observational studies, and case series with ≥10 participants were included, covering neuropsychiatric conditions such as OCD, treatment-resistant schizophrenia, and chronic anorexia nervosa. The primary outcomes were changes in clinical scales (e.g., PANSS, Y-BOCS) and adverse events, analyzed using critical appraisal tools such as RoB2 and the Newcastle-Ottawa scale.
Results
Out of 3351 initial records, 11 studies with 235 participants were included. Significant improvements were observed in specific symptoms: a 40% reduction in motor tics (p < 0.001) in Tourette syndrome, and a 10% increase in body mass index (p = 0.02) in anorexia nervosa. However, the effects on Alzheimer’s disease were heterogeneous, showing cognitive decline in patients <65 years (p = 0.006). Adverse events included mild neuropsychological impairment and severe perioperative complications in isolated cases.
Discussion
DBS proves effective in refractory neuropsychiatric disorders, modulating specific symptoms and improving quality of life. Methodological limitations persist in the literature, such as small sample sizes and heterogeneity in stimulation parameters. The need for multicenter studies and biomarkers to predict therapeutic responses is emphasized.