Objectives
1) to characterise clinically, neurophysiologically and manometrically the overactive bladder (OAB); 2) to objectify the lack of habituation in OAB; 3) to quantify the comorbidities associated with CS (central sensitisation); and 4) to evaluate the effect of neuromodulation (NM) of the tibialis posterior nerve in OAB.
Material and methods
Forty-seven patients, retrospective observational pre-post study.
Intervention: manometric biofeedback and posterior tibial transcutaneous NM (PTNM), 8 sessions.
Outcome variables: a) clinical (daytime urinary frequency [DUF] and nocturnal urinary frequency [NUF]), b) neurophysiological (latency, amplitude and percentage of habituation); c) comorbidities associated with CS; d) manometric (maximum and average pressure); at the beginning/end of treatment.
Results
Age, 58.91 ± 13.27 years. Comorbidities associated with CS, 1.98 ± 0.32 (range 1–5 pathologies). Percentage of habituation, 88.6%. PTNM decreased DUF (10.4 ± 4.86 to 6.21 ± 1.87 episodes; P = .0001), and NUF (3.02 ± 1.66 to 1.17 ± 1 episodes; P = .0001). PTNM increased maximum (38.46 ± 23.06 to 42.61 ± 19.46 mmHg; P = .0964), and mean (7.63 ± 3.56 to 8.66 ± 4.76 mmHg; P = .1639) pressure. NMTP modified latency (1.32 ± 0.32 to 1.38 ± 0.32 s; P = .3397), and reduced amplitude (1.98 ± 1.28 to 1.67 ± 1.44 mV; P = .0004) and habituation (88.6 ± 23.5% at 70 ± 30.2%; P = .0001) of sympathetic skin response (SSR).
Conclusion
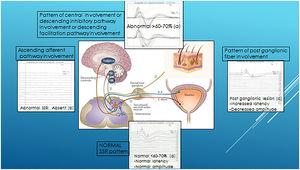
The lack of habituation is a neurophysiological phenomenon present in OAB. PTNM improved clinical and neurophysiological variables. SSR is a neurophysiological test capable of objectifying lack of habituation and could characterize other response patterns (alteration of the ascending, central, descending or postganglionic pathway).
