Introduction
The diagnosis of chronic obstructive pulmonary disease (COPD) requires the demonstration of poorly reversible airflow obstruction (defined by a forced expiratory volume in 1s [FEV1]/forced vital capacity [FVC] ratio <0.7 post-bronchodilation) in the appropriate clinical context (risk factors and exposures). Nevertheless, some individuals, who may be labeled “pre-COPD”, can present respiratory symptoms, structural lung abnormalities (e.g., emphysema), or other physiological abnormalities (e.g., low FEV1 [preserved ratio impaired spirometry, PRISm], gas trapping, hyperinflation, reduced lung diffusing capacity of carbon monoxide [DLco] and/or rapid FEV1 decline), all in the absence of airflow obstruction. For reasons that are still unclear, some – but not all – patients will eventually progress and develop airflow obstruction (i.e., COPD) over time. The aim of this study is to investigate the clinical, physiological, radiological and/or biological factors that are associated with progression from pre-COPD to COPD.
Material and methods
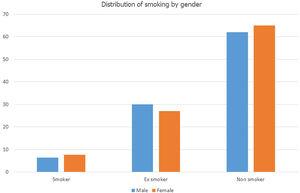
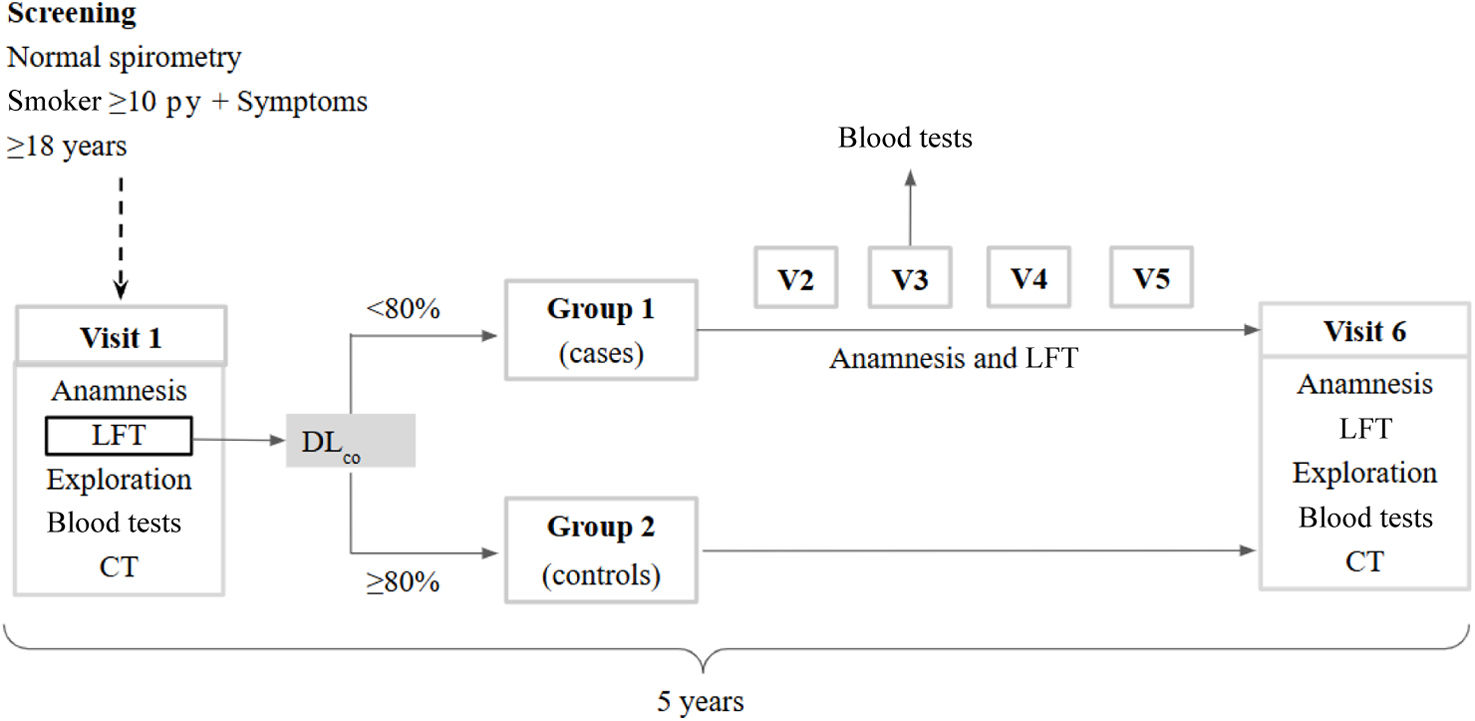
This will be a prospective (5-year follow-up), multicenter (conducted in 12 Spanish centers across eight geographical autonomous communities), observational, comparative study (www.clinicaltrials.govNCT04409275), that will recruit 285 current or former smokers (≥10 pack-years) with respiratory symptoms (dyspnea, chronic cough, sputum production, wheezing or recurrent lower respiratory tract infections) and spirometry without obstruction (pre-COPD status). Multivariate regression analysis and other tests will be used to analyze results.
Conclusion
Results are expected to provide novel, useful information for identifying pre-COPD individuals who are likely to develop progressive airflow obstruction and are potential candidates for prompt intervention.